(This is my story. It’s taken from my blog, mybumpandgrind.blogspot.com, which chronicled my pregnancy in the Netherlands, where home birth is the norm.)
There are few absolutes when it comes to labor. There’s no way to know just when it will start, how long it will last, or how it will feel. But one thing that I think applies universally is a quote from midwife Suzanne Stalls: labor is hard work, it hurts a lot, and you can do it.
Even with labor being so unpredictable and with no two labors being exactly alike, while pregnant I loved hearing other people’s birth stories. For me, labor has always been clouded in fear and mystery, and even though learning how it went for someone else told me nothing about how my labor would go, it was still reassuring to know it could be endured.
Of course it’s always nicer to hear the stories of relatively easy labors, but even the tougher experiences are promising, because they echo the most important part of what Suzanne Stalls says: labor is doable.
For me, labor was intermittent and gradual, and therefore quite manageable. Twenty-four hours passed between the contraction that was convincing enough to take seriously and the final push that brought it all to a close. That may sound long, but although labor was exhausting and all consuming in the last hours, for the most part it was what happened in the background, an interruption that came and went throughout an otherwise busy day.
On the day I went into labor, the Irish fella and I were frantically calling around looking to replace house cleaners who had failed to show. Weeks of construction in our new home had been completed the day before, and movers were scheduled for the next day. Months of living out of suitcases were coming to an end, but before we could move into our new house, we had to rid it of the dust, muddy boot prints, and general filmy filth that you’d expect at a construction site.
I had been having strong cramps throughout the morning and, at a scheduled midwife appointment, had been told that if I wanted to have my baby in the new house, I really ought to move that day. I met up with the Irish fella for lunch and I mentioned this as casually as I could, reminding him that it is common for women, particularly with their first pregnancy, to think they are in labor when they are not. This is false labor, I assured him, both because I believed it and because actually going into labor that day didn’t really suit our plans.
After a morning-long search, the Irish fella had found two cleaners to work on our house that evening. We made a list of supplies we needed and planned to spend the afternoon doing a preliminary scrub before the professionals arrived. Before setting off to buy mops and brooms and bleaches and detergents, the Irish fella suggested we time my cramps, which were twenty minutes apart.
We walked around a hardware store and a supermarket. We went to the house we’d been staying in and packed up some things we’d need for our first night in our new home. By the time we got to the new house, I was having cramps every ten minutes.
In my antenatal class, it was drilled into us that the best thing you can do in labor is stay upright, forward, and mobile. The Irish fella, for whom standing still is anathema, was all for my being active in labor. He handed me the vacuum.
We cleaned for a while, and my cramps, which we were now calling contractions, had intensified and were occurring every five minutes. The idea of being upward, forward, and mobile is to help things progress, but what I wanted then was to slow it down. I decided to rest.
The house was mostly empty, but we had one room that was furnished and decorated, with paintings hanging and new sheets on the bed, with books on the shelves and towels neatly folded on the side table. The Irish fella had put this room together before the construction work began, as a sort of shrine to normalcy. I was grateful for a bed to climb into.
The cleaners arrived and scrubbed the house around me. The Irish fella came to check on me from time to time, and we wondered whether we should cancel the movers we’d booked for the morning. The contractions intensified, and by 8 pm we called the midwife. At this stage, we really just wanted someone to tell us if I was actually in labor. We were still living in the reality in which moving house was the priority, and wanted to know if we should transition fully into the reality of my being in labor.
The midwife kept me on the phone long enough to hear me through a contraction. She said I sounded fine (“You are not screaming”) and to call her back in the night. We called the instructor from our antenatal class, asking her if she thought it’d be better for me to get up and move around or stay in bed. She said I could have hours or days to go. She told me to have a glass of wine and go to bed.
Labor is often compared to marathon running. Having now experienced both, I agree that there are similarities: both require endurance, mental and physical strength, controlled breathing, and regular hydration and energy repletion. Both also require proper pacing, which is where the analogy falls apart.
When you are running a marathon, you know exactly where you are in the race–you know how far you’ve gone and how far you have to go. In labor, you don’t, and having contractions for ten hours only to learn you are 1.5 centimeters dilated is akin to thinking you are nearly at the finish line when you are still doing warm-up laps. And not knowing how much more intense contractions are going to get can frighten women who are managing quite fine into receiving pain medication that they may, if they choose, do perfectly well without.
The Irish fella and I settled into bed. The contractions continued to come every five minutes, lasting for one minute, and getting stronger as the night went on. I got through each by exhaling deeply for a count of ten, inhaling deeply for a count of ten, and then repeating three times until the minute had passed. I reminded myself that each contraction was getting me closer to meeting my baby. On occasion I heard myself asking God or my mom for help.
The Irish fella and I had a hot water bottle between us, and throughout the night we’d press together to push it as hard as we could against my lower back during contractions. I didn’t sleep, but I managed to doze during those five-minute spells when there was no discomfort at all. I considered calling the midwife again around 3 am, but when I envisioned her arriving and the lights going on and the atmosphere changing, I decided to wait.
At 8 am we sat in bed and discussed what to do. Should we call the midwife? Should we cancel the movers? If I was only in the very early stages, we reasoned, I could have a good twelve hours to go, in which case we may as well have our furniture moved. We called the midwife, hoping she’d come examine me, and expecting she’d say I was maybe at two centimeters, in which case we’d stick to our moving plan.
When the midwife arrived, we waited for a contraction so she could feel my cervix. I breathed deeply–ten seconds out, ten seconds in, repeat–and when I opened my eyes she was removing her rubber glove and smiling. “Nearly seven centimeters,” she said. “I can get you through this.” She told the Irish fella he should go out for a walk, get a coffee, and come home in about an hour. She suggested I get in the bath. We rescheduled the movers.
It was a huge relief to know that I was not only definitely labor, but that I was actually quite far along. We were all delighted. The midwife brought in her birthing stool and prepared the bed with rubber sheets. The kraamzorg arrived–the nurse who would attend the birth and care for me after–and set out clothes for the baby. I apologized over and over for not having any furniture for them to sit on, and for the general state of the house.
I also apologized each time I felt a contraction coming, because it was impossible to concentrate on anything else in the midst of one. But between contractions, I was myself, and with a heightened politeness. The mood was so pleasant and the two women who buzzed around me while I floated shamelessly in my bathtub were so friendly that we were, dare I say, having a nice time.
There was laughter and small talk and banter, and then every five minutes, I would morph into some primal version of myself–not a werewolf perhaps, but some form of lowing, moaning creature. Once a contraction was over, I’d return to the conversation until the next one started.
The Irish fella returned. At 11 am, I got back on the bed, and the midwife suggested she break my water to speed things up. I couldn’t see anything over my enormous bump, but I heard her ask the Irish fella if he saw what color the warm liquid was. “Green,” he said. “Erwtesoep,” she said. Pea soup. “And what does this mean?” she asked him, instructor to student, and he answered, “We have to go to hospital.”
The green color of the water is a sign that there is meconium, the baby’s first feces, in the amniotic fluid. Breathing this can be harmful to the baby, and its presence is a sign that the baby is stressed. Although the midwife was monitoring the baby’s heart and it sounded fine, a more accurate method of heart monitoring–whereby a monitor is physically clipped to the skin on the baby’s head–can only be done in the hospital. By law, we had to move.
At 8 centimeters with the end just in reach, getting up, putting jeans on, walking to the car, and driving to the hospital was the last thing I wanted. And I’d like to extend sincere apologies to the poor man with whom I held mid-contraction eye contact while stopped at a red light. But within 15 minutes, I was in a hospital bed ready to resume.
But everything was different, and I think it shut my labor down. The midwife had to leave so the doctor could take over. The heart monitor meant I couldn’t move around anymore, no more shower or bath. I still had my hot water bottle, which the nurse wanted to take from me because it was giving me burn blisters, but I wouldn’t give it up.
Two hours passed and I was still at 8 centimeters. The doctor explained that they would like to give me a drug that helps speed up contractions. So ingrained is the belief in natural childbirth in the Netherlands that even this relatively minor intervention was explained to me with reassurance that it was nothing I was doing wrong, that I was still doing all the work, but that they had to do this to help move things along, to help me.
Things were harder now. The drug sped contractions up so I was now having four every ten minutes, and they were far stronger. We were left alone, and the Irish fella sat next to me and rubbed my shoulders while pressing the hot water bottle into my back. When a particularly hard contraction had me hyperventilating, he would breathe deeply until I was back on course by following his pattern. But in between contractions, there were kisses, there were jokes about the faces I was making, there was a phone call about the delivery of our new dining room table. In between, I was tired and thirsty, but I was fine.
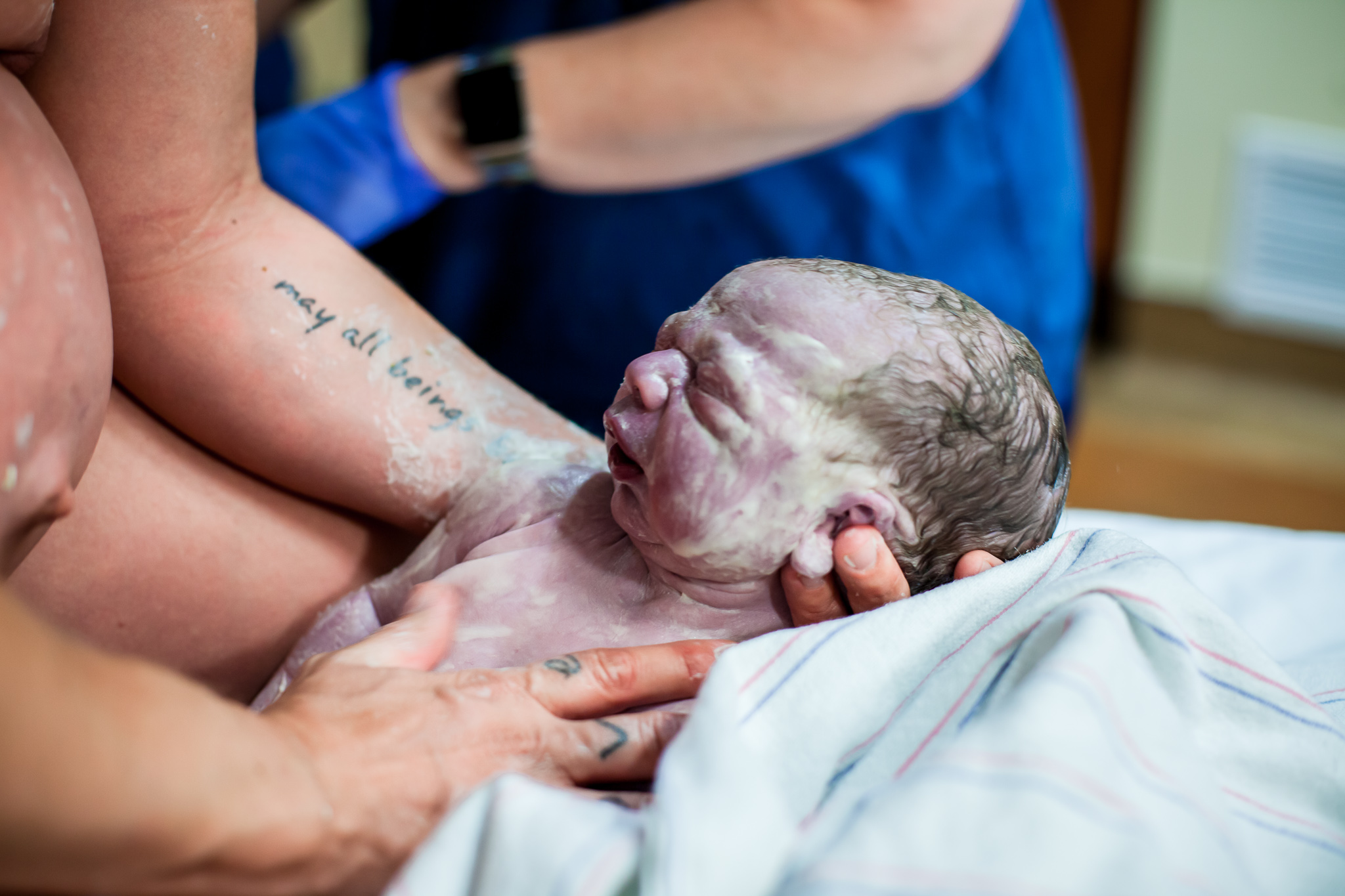
When I was at ten centimeters, the doctor said I was ready to push. In spite of it being 24 hours since I put down the vacuum and climbed into bed, when the doctor said it was time I heard myself say, “already?” And so there I was, in the hospital, knees to ears, Irish fella to my left, doctor, nurse, and intern at my legs, waiting for a contraction so I could push. In three pushes, my baby was resting on my chest.
It’s a bit of a blur, those first minutes. The Irish fella cut the cord. The doctor and intern and nurse took the baby to a table to examine him, and the Irish fella followed them. I stayed on the bed, streaked with sweat and blood. My belly was a soft, empty pouch. I was dying of thirst but my Powerade was just out of reach, and not a person in the room was paying any amount of attention to me. From a tray across the room, the placenta seemed to say, “Tell me about it, sister.”
It was all over and I felt fantastic. One benefit to drug-free labor that I appreciated right away was that I could walk around, and felt no grogginess. My baby was placed on my chest and began to feed. The physical pain of contractions was gone, and the elation of knowing my baby and I made it through labor happy and healthy made it all worth while. They say women forget the pain, but I don’t think that’s it. I remember it. And as soon as it was over, I remember thinking it was not at all worth fearing. It wasn’t that bad, and it was definitely worth it.
For the last week I’ve been hearing the birth stories of the women from my antenatal class, and some of them had labors that were far longer and harder than mine. Still, we have all said it is something we know we want to do again. We know it will be hard work and it will hurt, but we also know it will be manageable, completely worth it, and most important, we know we can do it.



+ show Comments
- Hide Comments
add a comment